Revenue Cycle Management (RCM) is a major function of medical practice.
This system runs as the health facilities’ bloodstream.
Without proper functional Revenue Cycle Management, hospitals and clinics will face major problems in cash flow.
Thus, with a strategically managed RCM, medical billing errors will reduce, and reimbursements will be maximized.
Overall, the RCM cycle in medical billing is crucial for every healthcare organization’s survival in the competitive space.
The healthcare systems are focusing on advancements to improve their revenue flow.
Today, above 66% of healthcare organizations have switched to automation to run their revenue cycle operations.
The global RCM market reached a valuation of $109.5 billion in 2021. It is further expected to reach $367.7 billion by 2031.
Innovative approaches have led to the strategic management of RCM.
This article will give you a clear insight into RCM and its importance in the healthcare system.
Dive into the below sections to learn about this system, starting from the basics.
What is RCM in Healthcare?
Revenue cycle management (RCM) in healthcare is the financial process of managing the cash flow and effective billing process.
In today’s digital era, healthcare organizations have shifted to medical billing software for RCM.
It aids in tracking every episode of patient care, starting from registration to final payment.
RCM helps in unifying the business and clinical sides of the healthcare system.
It brings administrative data such as the patient’s name, insurance provider, and other personal information.
The RCM cycle in medical billing starts when the patient schedules an appointment to seek medical treatment.
The cycle ends when the healthcare organization collects all claims and payments of the patients.
However, the patient’s account is not as simple as it seems.
By keeping up with the best RCM services, healthcare organizations can commit to meeting the patient’s expectations.
Effect Of COVID-19 Pandemic on RCM
According to the reports of HFMA – Healthcare Financial Management Association, the COVID-19 healthcare systems have reported that the variable volume of claims was one of the biggest alarming issues.
The rising number of patients in healthcare centers has led to confusion in the billing process.
Due to improper coding guidelines, the billing professionals faced serious problems and complained of increased workloads.
Many organizations have noticed a severe decrease in staff productivity.
Moreover, the staff shortage was another underlying problem in the healthcare facilities during the period.
The revenue cycle professionals stated that improper RCM and an increase in staff reductions led to a major decrease in productivity.
Integration of Automation in RCM
According to the survey, automation in revenue cycle management in hospitals has noticed a 12% increase.
Compared to the pandemic days, the integration of automation in the RCM cycle in medical billing has reached a massive height.
The survey program is based on data collected from around 400 chief financial officers and revenue cycle leaders in healthcare settings in the USA.
The HFMA’s Pulse Survey program inspected the responses in the months of May and June 2021 and published the reports.
The rise in automation in RCM was the result of the COVID-19 pandemic’s effect. It has brought forward unstable claim volumes and heavy workload complaints to the forefront.
Healthcare systems adopted prompting revenue cycle automation technology to deal with such emergencies in the near future and strengthen the revenue cycle.
The automation process has improved the workflow and reduced manual pressure and errors. The integration has also minimized the overall costs in healthcare settings.
It has also streamlined the accounts payable, receivable transactions, billing, payment posting, and reimbursements.
It has successfully eliminated human error due to manual entry.
It has resulted in highly accurate RCM. Due to the higher adoption rate of automated RCM processes, in the coming years, more advancements will be brought to the system.
It has also led to the integration of Artificial Intelligence, which has fastened and strengthened the RCM cycle steps.
Therefore, sheer improvement is now noticed in the medical billing process compared to the past decades.
Advantages of Integrating Strategic RCM in Healthcare System
When the healthcare organization makes a decision to integrate a strategic RCM process in the billing process, it comes with a lot of benefits to boost business performance.
Also, it results in delivering the best quality service to the patients.
Here are the advantages of a well-functioning RCM cycle system in the healthcare facility.
Highly Streamlined Process Than Ever Before
The billing process will be more streamlined than your traditional method.
The automated process will enhance the revenue cycle management steps.
It will offer health professionals and coding specialists safer access with a simplified solution.
The staff will get rid of all the hassles and time-consuming processes.
An excellent system will eventually reduce the errors making the process more accurate.
It will relieve the staff from all kinds of confusion and frustration with large bills.
The whole process, from registration to claim submission, will be automatically streamlined.
Improves Patient Experience with Great Service Features
A well-functioned system and a highly skilled team will transform the coding and billing process more efficiently.
Automation will result in a seamless RCM cycle diagram.
The entire RCM steps will be made more feasible than before.
The strategic system involves simplifying the operational process.
It will also improve the patient interaction points at every step. This will make the patients less worried, which results in great customer support.
Further, it will improve the quality of care in healthcare facilities.
The integrated RCM process will result in patients receiving better care, and the staff will get enough time to devote to their patients.
Fewer or Zero Denials of Claims
Denials are often the result of errors in the claims. When the RCM is pressurized with heavy workloads, it leads to manual errors in the data input.
This becomes the major reason behind denials.
This is where your organization needs a fully optimized revenue cycle management system.
A properly optimized system will reduce the chances of error.
It will ensure the claims are error-free and accurate before the final submission.
It will eventually reduce claim denials and speed up reimbursement processes.
This will keep your healthcare business profitable and make your service more trustworthy.
13 RCM Cycle Steps in Medical Billing
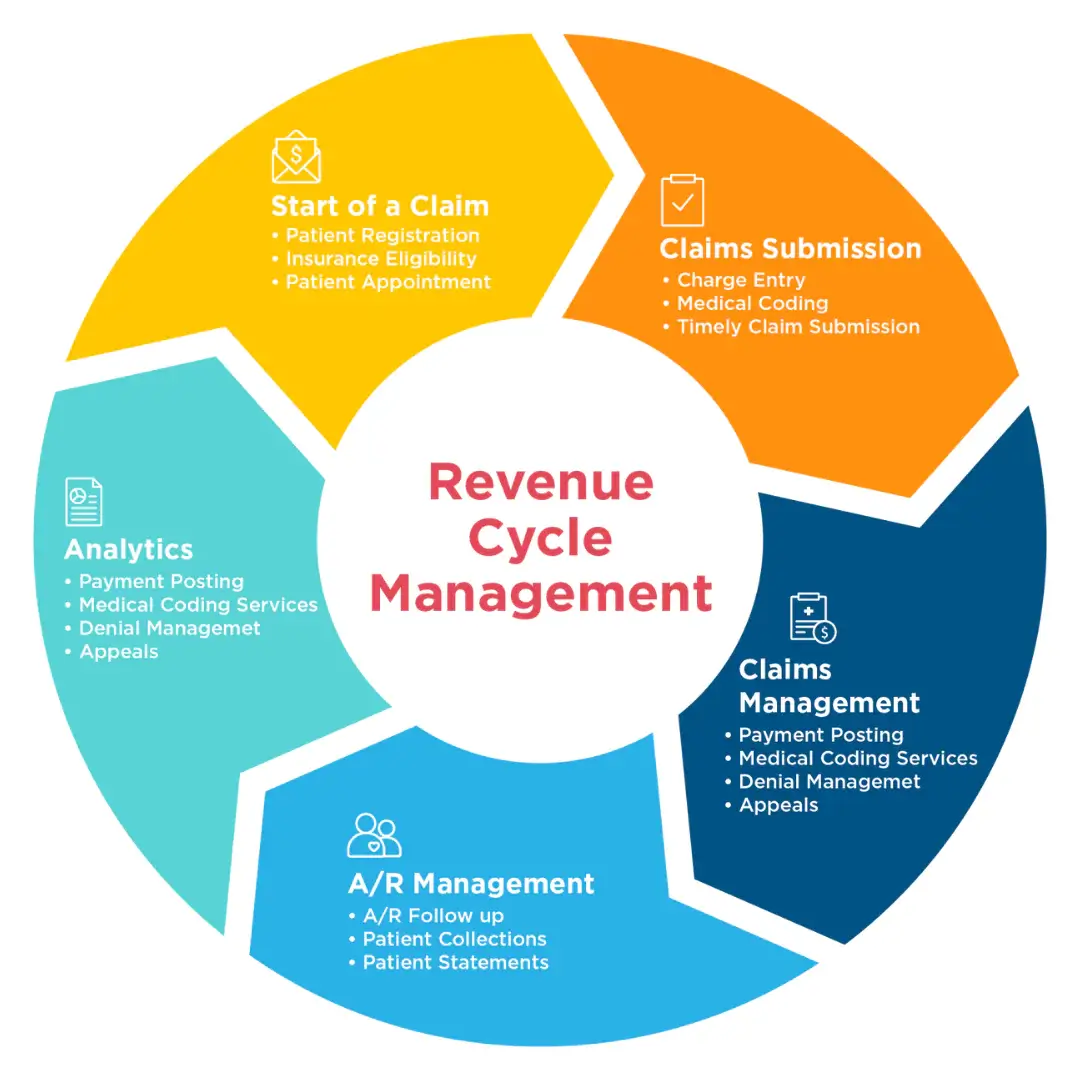
Do you know how many steps in RCM cycle? Here we brought you the complete revenue cycle steps in detail.
- Preregistration of Patient and Insurance Eligibility
Preregistration is the foremost step in the revenue cycle process.
This process captures the patient’s demographic and insurance information.
This data reaches the patient’s insurer and further flows through the provider’s system.
It states the insurance provider about the medical expense coverage, co-insurance, co-payment, deductible, and other information.
- Registration
This process solidifies that the patient’s information is accurate.
Here, the service provider ensures all information related to the patient, such as their address, contact number, DOB, and insurance information, are 100% true.
This information is safeguarded and secured whenever the patient is treated.
- Capturing Charges
Capturing the charges is another major revenue cycle process.
Due to an inclination towards automation technology, the charges are now automatically captured, directly flowing into the system.
Some organizations still follow the old technique of manual data entry at the front desk, which is sent to the billing section.
- Utilization Management
In the utilization management process, the health insurance providers will examine the request received for the medical services to be covered.
The utilization purpose will be confirmed and approved if the health care plan covers the claimed medical services.
The insurer will also ask the hospital to reduce the charges.
- Medical Coding
It is a crucial part of converting medical diagnoses and procedures into alphanumeric and numeric codes.
The medical services, requirements, and processes the patient undergoes are programmed and translated into codes.
The billers utilize the codes to develop bills and claims for the patients and service providers.
- Verification of Eligibility and Benefits
The claims need to be verified to confirm their eligibility and benefits.
With the rightly managed RCM process, the services can easily process eligibility verifications.
Integration of automation will clear out the billing errors and efficiently manage delayed payments and the reason behind payment failure. In this process, periodic checks take place.
- Submission of Claims
This medical billing RCM cycle process involves sending information to the insurance provider after the charges are successfully entered into the billing section.
Here, the RCM team plays a major role in looking after the charges along with the CPT and the diagnosis code.
The team will check whether the diagnosis supports the procedure or not. In case multiple services are included, the expenses are separately coded.
- Processing Remittance
The next major step in RCM is processing remittance. Once the practice is successfully claimed, it will get back the remittances.
In this process, acceptable claims are determined.
Here, the allowable provided by the service provider is contracted with the insurer.
Then the provider and insurer negotiate the claimed contract.
The insurance company will check the transferred data and confirm what charges or expenses will be covered for each medical service performed.
- Denial Management
Management of denials is the most important in the RCM process.
Here, the payments are either rejected or accepted after the claims are verified.
The staff will verify and analyze the received payments from the insurer and check out whether they can be approved or if there are any discrepancies that can be the reason behind delayed payment.
If any error is found in the claim, it will be directed back to the clearinghouse, where it will be assessed and cleared.
- Insurance Follow Up
Insurance follow-up is the crucial step of the medical billing RCM cycle.
Here, the practices check what can be covered under the insurance and what cannot be paid.
The A/R – accounts receivable report details the charges covered in the insurance. This report will show whether the follow-up is broken or why it is time-consuming.
- Patient Collections
This is the final part of the RCM process but also the most problematic part. This should be processed strategically.
This is why the front desk staff are trained to collect during service time.
The healthcare organization must prevent the backlog from snowballing.
The team should ensure they are following the standard policy and practices to collect the co-payments and deductibles to meet the financial expectations.
- Cash Posting
In the process of cash posting, the staff identifies the potential issues and addresses them.
It gives a view of the payments made for the treatment with a clear insight into the financial practices.
After this process is followed right, it plays a vital role in the development of RCM. It finally aids in driving the revenue rate.
- Reporting
This process is a major step in the RCM cycle to filter out costly mistakes.
A top-notch quality reporting technology will be very helpful.
Therefore, when you adopt a high-quality technological aid for proper reporting, minor to major mistakes can be effortlessly identified and fixed immediately.
Factors Affecting Healthcare Revenue Cycle
A precisely managed medical revenue cycle management system leads to building strong bonds with patients.
But, when you observe your healthcare service is lacking behind, there may be some underlying factors affecting the revenue cycle.
Also, there will be factors affecting medical billing and coding.
To understand what things are affecting your revenue loss in your healthcare practice,
you have to understand the possible factors that cause financial damage.
Check out the below factors in detail.
Inaccurate Patient Information in the Records
The medical revenue cycle begins with medical billing.
It further starts with patient encounters. The billing staff must gather all the information accurately.
If incorrect information is mentioned, the billing procedure won’t function smoothly.
With accurately mentioned information, it will prevent delays and redundancies in claims.
At times, errors in health insurance, such as patient eligibility not being recorded accurately, takes longer time to fix.
This impacts the complete revenue cycle management of your business.
Credentialing and Enrolment Failure
The billing and coding team must be very careful while updating the credentials.
A minor error in the credentials can greatly impact future results.
Some healthcare practices ignore on-time enrolment and updating the credentials. Specifically, in the case of new users, these issues take place.
This further results in claim denials and reimbursements, delayed payments, and out-of-network or nonfunctional services.
All these things will further lead to revenue loss.
Therefore, it is crucial to keep the credentials updated regularly.
Mitigating Claim Denials
The common issue faced by healthcare practices is claim denials.
It brings a huge negative impact on the revenue cycle.
Claim denials are not only due to single reasons. There are multiple factors associated with claim rejection.
Errors in medical coding, duplicate claims, lack of accurate or missing information, on-time failure claim, etc., lead to claim rejection.
The complete billing team should be aware of these factors before proceeding with the claims.
Follow-up of each claim is necessary, and it is important to know the reason behind the rejection.
Manual Record Keeping
The complete medical billing and coding system is way too complex than it seems.
And some organizations still follow the traditional manual method of record-keeping.
Manually entering the billing details and claims are considered inappropriate due to the higher possibility of errors.
The manual process builds room for many mistakes that eventually affects the RCM.
This is why healthcare technologies are now upgraded with automation.
Automating the record-keeping process will reduce errors and improve efficiency.
Moreover, there will be less stress on the billing team.
It’s high time for healthcare practices to go for the right software and automation methods to process bills and claims.
Lack of Tracking Financial Performance
Most revenue loss issues arise due to the lack of tracking financial performance.
When you wish to maintain a successful practice, it is necessary to regularly monitor the performance.
And to track it in the right way, the healthcare facility must analyze the KPIs.
Moreover, they should keep an eye on the factors leading to revenue leaks.
It will further result in maintaining consistency in cash flow.
It is an appropriate way to get back on track.
The organization can make a decision to outsource its medical billing and coding to track the essentials.
Final Thoughts
Transform your revenue cycle management process and take it to an advanced level with automation. There are many automated and streamlined RCM billing services available to aid hospitals and clinics. In the future, with the integration of cloud-based RCM deployments and artificial intelligence, the billing process is going to become more instant and efficient.



















